The problem was discovered during routine FSIS surveillance activities of imported products, and it was determined that the products were not presented for reinspection.
FSIS is concerned that these products may be available in retailers’ deli counters and available for consumers to purchase. Also, these products may be in retailers’ freezers.
The recalled items were shipped to retail locations in California.
Recalled products:
- 19- to 24-lb. box containing “Chicharrón con carne/Pork Skin with Meat” with lot codes 2193CON0281, 2203CON0283, 2213CON0285, 2223CON0287, 2233CON0289 and use by date between August 7-11, 2024, and shipping mark 176.
- 24- to 30-lb. box containing “Carnitas de Cerdo/Seasoned Pieces of Pork Meat” with lot codes 2123CON0272, 2133CON0273, 2193CON0282, 2203CON0284, 2213CON0286, 2223CON0288, 2233CON0290 and use by date between July 31, 2024-August 1, 2024, and between August 7, 2024-August 11, 2024, and shipping mark 177.
The products subject to recall bear Mexican establishment number “TIF No. 681” inside the Mexican mark of inspection. Product labels can be viewed here.
As of the posting of this recall, there have been no confirmed reports of adverse reactions due to consumption of these products.
Retailers are urged not to serve these products. These products should be thrown away or returned to the place of purchase.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The study was conducted by scientists at the University of Pretoria (UP) in 2019 and 2020 into the prevalence of Listeria monocytogenes in beef and beef products at abattoirs and retailers in the Gauteng, Mpumalanga and North West provinces.
It showed that 4.6 percent of chilled carcasses sampled at seven abattoirs in Gauteng were positive for Listeria. This means that contaminated items could enter the food chain as beef products sold at retail outlets in the province.
The study, funded by Red Meat Research and Development South Africa, was prompted by the 2017-2018 outbreak of listeriosis with 1,065 confirmed cases and 218 deaths. It was traced to a ready-to-eat processed meat product called polony, made at a plant in Polokwane run by Enterprise Foods, which at that time was owned by Tiger Brands.
Ready-to-eat (RTE) food, including polony, were also positive for Listeria in the current study.
Supply chain assessment
“Processed foods become contaminated by contact with equipment, the handling of raw products, or from post-processing settings in which the pathogen can survive despite the routine use of disinfectants. Because of potential contamination during slaughter, carcasses can become contaminated, leading to contaminated meat and meat products,” said Dr Rebone Moerane, head of UP’s Department of Production Animal Studies, who was part of the research team.
Another study, published in the Journal of Food Safety, revealed that 8.3 percent, or 33 of 400, beef and beef products were contaminated with Listeria monocytogenes.
University of Pretoria researchers also looked at the prevalence and factors associated with Listeria in cattle, silage, feeds, and water on farms in the three provinces; in slaughtered cattle and carcasses at processing plants; and the contamination of beef products at retail.
Samples were collected from cattle farms; carcass swabs were taken from abattoirs, and samples of raw beef and beef products, including ready-to-eat items, were collected from shops of all sizes.
Researchers found the risk of exposure of cattle to listeriosis on farms is minimal. However, the detection of contaminated chilled carcasses sampled at Gauteng abattoirs is troubling, as are the findings at retail outlets, they said.
Get ahead of another outbreak
The prevalence of Listeria was 6 percent, 8.3 percent, and 9.3 percent in beef and beef products sampled in outlets in North West, Mpumalanga, and Gauteng respectively, and 4.3 percent, 11 percent and 9.3 percent for cold beef and beef products.
“Some of the contaminated products were RTE items – including polony, which is widely consumed, and biltong. This increases the risk of human exposure to the pathogen,” said Dr. Moerane.
“It’s our hope that government and industry stakeholders will act on these findings and introduce strict control and monitoring measures at the appropriate stages in the beef production system. It’s vital that we use the outcomes of this study to get ahead of another potential outbreak of listeriosis.”
In most cases, Listeria monocytogenes isolates responded to penicillin, ampicillin and sulfamethoxazole-trimethoprim, which are important antimicrobials used to treat listeriosis.
Scientists recommended that government and industry implement stringent food safety measures at abattoirs and processing plants to reduce contamination and lower the possibility of another listeriosis outbreak.
They also suggested follow-up studies of moist biltong, which is widely consumed in the country, to determine its ability to support the growth of Listeria and assess the risk posed to consumers.
(To sign up for a free subscription to Food Safety News, click here.)
]]>On Sept. 5, 2023, the firm was notified by the South Carolina Department of Health and Environmental Control (SCDHEC) that their Not Fried Chicken ice cream treat tested positive for Listeria monocytogenes. The firm also recalled their Life Is Peachy Ice Cream treats because both products were manufactured in the same room.
These products were packaged in lamented buckets and plastic wrap and shipped to Georgia, Illinois, Maryland, North Carolina, New York, South Carolina and Texas distribution centers. The product was also shipped online directly to consumers located in all fifty states plus the District of Columbia.
Recalled products:
| Product | Size | UPC | Use By Dates |
| LIFE RAFT TREATS LIFE IS PEACHY | 6 COUNT | NO UPC CODE | Up to andincludingBEST BYAUG 8212024 |
| LIFE RAFT TREATSNOT FRIED CHICKENICE CREAM | 64 OZ BUCKET | NO UPC CODE | Up to andincludingBEST BYAUG 8212024 |
| LIFE RAFT TREATSNOT FRIED CHICKENICE CREAM | 2.5 OZ BAR | 8 60006 18210 6 | Up to andincludingBEST BYAUG 8212024 |
As of the posting of this recall, no illnesses have been reported to date.
Consumers who have purchased these products are urged not to consume them and to return the products to the place of purchase for a full refund or they may discard the product.
About Listeria infections
Food contaminated with Listeria monocytogenes may not look or smell spoiled but can still cause serious and sometimes life-threatening infections. Anyone who has eaten any recalled products and developed symptoms of Listeria infection should seek medical treatment and tell their doctors about the possible Listeria exposure.
Also, anyone who has eaten any of the recalled products should monitor themselves for symptoms during the coming weeks because it can take up to 70 days after exposure to Listeria for symptoms of listeriosis to develop.
Symptoms of Listeria infection can include vomiting, nausea, persistent fever, muscle aches, severe headache, and neck stiffness. Specific laboratory tests are required to diagnose Listeria infections, which can mimic other illnesses.
Pregnant women, the elderly, young children, and people such as cancer patients who have weakened immune systems are particularly at risk of serious illnesses, life-threatening infections, and other complications. Although infected pregnant women may experience only mild, flu-like symptoms, their infections can lead to premature delivery, infection of the newborn, or even stillbirth.
(To sign up for a free subscription to Food Safety News, click here.)
]]>According to the details posted online by the FDA, the recall was initiated on June 16, 2023, and is ongoing.
The recalled products were distributed in Illinois, Alabama, Iowa, Georgia, Mississippi, Indiana, Arkansas, Colorado, Florida, Virginia, Ohio, Wisconsin, Pennsylvania, New Hampshire, Arizona, Kansas, Texas, Tennessee, North Carolina, Lousiana, Missouri, Kentucky, Delaware and Wisconsin.
Recalled products:
Parent’s Choice brand Sensitivity Premium Infant Formula
- 638g
- packaged in plastic tubs
Tippy Toes brand Sensitivity Premium Infant Formula
- 942g
- packaged in composite cans
Code information:
- D05LVJV
- USE BY 05MAR2025
- D06LT7VA
- USE BY 06MAR2025
UPC Codes: 36800496644 and 681131045513
Anyone who purchased the recalled products should immediately dispose of it and not consume it.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Nineteen sick people are aged 63 to 93, including 13 men and six women. Patients have been reported from 10 different regions.
Six people with listeriosis have died. However, it is unclear what role the infection played in their death because most patients had other severe underlying diseases.
People have been sick with the same type of Listeria since autumn 2022, but 15 cases occurred from the end of May this year, said Folkhälsomyndigheten (the Public Health Agency of Sweden).
Of cases with available information, 14 reported eating vacuum-packed salmon from one of two brands before falling sick. Both these brands are produced by Leröy Seafood, and Listeria was detected in products and environmental samples in the firm’s facility.
In most cases, samples have only been analyzed qualitatively so it is unclear if Listeria was above the limit of 100 CFU/g, according to Livsmedelsverket (the Swedish Food Agency).
“For Leröy Smögen Seafood, safe and secure food is our priority, and we take this incident very seriously. We are doing everything we can to ensure this does not happen again. We have a good cooperation and dialogue with the Swedish Food Agency,” said a company statement.
Finding the source of infections
Further analysis of samples from food, the environment, and human cases found the same type of Listeria, which points to the salmon products being the likely source of infection. The company has increased sampling and is carrying out further clean-up measures at the facility.
In early August, the retailer Axfood recalled a batch of Falkenberg Seafood cold smoked salmon 200-grams after low levels of Listeria were found.
The product was available for sale in the majority of Axfood’s stores. Listeria was detected during the retailer’s internal checks.
“The production has not been stopped, but all batches are currently analyzed for the presence of Listeria before release on the market. The company must take action following its HACCP-based procedures. They must also investigate the cause of contaminated products with Listeria monocytogenes and take measures to prevent such contamination. This may involve changes to HACCP-based procedures or other measures,” said Mats Lindblad from Livsmedelsverket.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The problem was discovered during routine FSIS surveillance activities of imported products, and it was determined that the products were not presented for reinspection.
The products subject to recall bear Canadian establishment number “391” inside the Canadian mark of inspection.
Recalled product:
FSIS is concerned that some products may be in consumers’, restaurants, and institutions’ freezers.
- 15-kg/33.07-lb. cases containing “Frozen Pork Front Hock” with case code 18019 and Cert. No. 251497 and best before dates between July 14-27, 2025.
As of the posting of this recall, there have been no reports of adverse reactions due to consumption of these products. Anyone concerned about a reaction should contact a healthcare provider.
These items were shipped to Hawaii and American Samoa distributors and exported to Palau.
Consumers who have purchased these products are urged not to consume them. Restaurants and institutions are urged not to serve these products. These products should be thrown away or returned to the place of purchase.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The Joint FAO/WHO Expert Meeting on Microbiological Risk Assessment (JEMRA) event, at FAO headquarters in Rome on Sept. 18 to 22, will work on food attribution, analytical methods, and indicators of viruses in foods.
United States-based experts proposed for the meeting are Donald Schaffner, of Rutgers University; Xiang-Jin Meng, at Virginia Tech; Kali Kniel, from the University of Delaware; Lee-Ann Jaykus, at North Carolina State University; and Jacquelina Williams-Woods of the FDA.
In 2022, the Codex Committee on Food Hygiene (CCFH) asked JEMRA to provide scientific advice to inform a review of guidelines established in 2012. This was due to emerging issues associated with foodborne viruses and scientific developments.
Aims of first meeting
The main purpose of the past document was to give direction on how to prevent or minimize the presence of human enteric viruses in foods, especially Hepatitis A virus (HAV) and Norovirus.
It was applicable to all foods, with a focus on ready-to-eat food, from primary production through to consumption.
The guide also contains an annex on the control of Hepatitis A virus and Norovirus in bivalve mollusks and the same two agents in fresh produce.
JEMRA’s work will focus on reviews of the foodborne viruses and relevant food commodities of the highest public health concern; the analytical methods for relevant enteric viruses in foods and of scientific evidence on the potential of viral indicators or other indicators of contamination.
Experts will also look at the scientific evidence on prevention and intervention measures and the efficacy of interventions.
The provisional list of 23 scientists also includes Magnus Simonsson, director of the European Union Reference Laboratory (EURL) for foodborne viruses; Shannon Majowicz, from the University of Waterloo; and Joanne Hewitt, at Environmental Science and Research in New Zealand.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Recent modifications to FDA’s import alerts, as posted by the agency, are listed below.
Click here to go to the FDA page with links to details on specific alerts.

(To sign up for a free subscription to Food Safety News,click here)
]]>The warning and related recall posted today by the Food and Drug Administration did not indicate a specific contaminant.
Restaurants and food retailers in Connecticut, Massachusetts, New York, Pennsylvania and Virginia that have recently purchased raw oysters from Groton Approved area in Connecticut harvested from Aug. 28 through Aug. 30 should not sell the oysters.
The oysters were directly distributed to retailers and distributors in Connecticut, Massachusetts, New York, Pennsylvania and Virginia. The oysters may have been distributed further from these states.
The implicated oysters are from Groton Approved area in Connecticut harvested by dealers CT-393-SS, AQ, CT-004-SS, AQ, and CT-020-SS, AQ with lots, L-30 and L-26B1.
On Aug. 31 the Connecticut Department of Agriculture, Bureau of Aquaculture initiated an emergency precautionary closure of two approved harvest areas and a recall of the implicated oysters because sample results showed potential contamination.
All impacted commercial harvesters agreed to recall the implicated oysters. The affected harvest area will remain closed until the source of contamination is identified and corrected, and the CT Department of Agriculture has collected acceptable sample results to reopen the area.
Contaminated oysters can cause illness, especially if eaten raw, particularly in people with compromised immune systems. Food contaminated with pathogens may look, smell, and taste normal. Consumers of these products who are experiencing food poisoning symptoms such as diarrhea, stomach pain or cramps, nausea, vomiting, or fever should contact their healthcare provider, who should report their symptoms to their local health department.
(To sign up for a free subscription to Food Safety News,click here)
]]>According to the details posted online by the FDA, the recall was initiated on Aug. 1, 2023, and is ongoing.
The recalled products were distributed in Nevada.
Recalled product:
- Ruby Mountain Spring Water 3 and 5-gallon plastic water jugs
- Product Quantity: 1,350 bottles
Anyone who purchased the recalled product should immediately dispose of it and not consume it.
(To sign up for a free subscription to Food Safety News, click here.)
]]>This voluntary recall is being issued because a sample of Victor Super Premium Dog Food tested positive for Salmonella in a random sample test conducted by the South Carolina Department of Agriculture.
The recalled dog food was produced at its Mount Pleasant, TX production facility.
Salmonella can affect animals eating the product and there is a risk to humans, notably children, the elderly, and the immunocompromised, when handling contaminated products, especially if they have not thoroughly washed their hands after having contact with the products or surfaces exposed to these products.
Dogs with Salmonella infections may be lethargic and have diarrhea or bloody diarrhea, fever, and vomiting. Some dogs will have only decreased appetite, fever, and abdominal pain. Infected but otherwise healthy dogs can be carriers and infect other animals or humans. If your dog has consumed the recalled product and has these symptoms, please contact your veterinarian.
Recalled product:
- The affected product was only sold in 5-pound bags.
- Products were distributed to various distributors and retailers in the United States.
- The affected product consists of 644 cases sold in 5-pound bags with lot code 1000016385 with Best By Date 4/30/2024.
- Lot code information is found on the back of the bag.
As of the posting of this recall, no human or pet illnesses have been reported.
Retailers and distributors should immediately pull the recalled lot from their inventory and shelves. Recalled products should not be sold or donated.
The recalled product should not be fed to pets or any other animals. It should be destroyed in a way that children, pets and wildlife cannot access. Pet food bowls, cups and storage containers should be washed and sanitized. Pet owners should always ensure they wash and sanitize their hands after handling recalled food or any utensils that come in contact with recalled food.
About Salmonella infections
Food contaminated with Salmonella bacteria does not usually look, smell, or taste spoiled. Anyone can become sick with a Salmonella infection. Infants, children, seniors, and people with weakened immune systems are at higher risk of serious illness because their immune systems are fragile, according to the CDC.
Anyone who has used any of the recalled products and developed symptoms of Salmonella infection should seek medical attention. Sick people should tell their doctors about the possible exposure to Salmonella bacteria because special tests are necessary to diagnose salmonellosis. Salmonella infection symptoms can mimic other illnesses, frequently leading to misdiagnosis.
Symptoms of Salmonella infection can include diarrhea, abdominal cramps, and fever within 12 to 72 hours after eating contaminated food. Otherwise, healthy adults are usually sick for four to seven days. In some cases, however, diarrhea may be so severe that patients require hospitalization.
Older adults, children, pregnant women, and people with weakened immune systems, such as cancer patients, are more likely to develop a severe illness and serious, sometimes life-threatening conditions.
Some people get infected without getting sick or showing any symptoms. However, they may still spread the infections to others.
(To sign up for a free subscription to Food Safety News, click here.)
]]>In late August, the National Health Surveillance System was notified of the cases following a meeting at a house in the district of Buenos Aires.
Three patients are adults and one is a child under 5 years old. All of them have been hospitalized and received treatment with antitoxin.
Investigations have revealed that all cases are related and shared, among other foods, some type of homemade preserve. Lab analysis identified botulinum toxin type A in one of the jars of this food.
Health officials said the early suspicion and notification of cases made it possible to quickly identify those affected, commence treatment and start the epidemiological investigation. This identified the homemade preserves as the source, which allowed potential further infections to be avoided.
Botulinum poisoning is a rare but life-threatening condition, caused by toxins produced by Clostridium botulinum bacteria. In foodborne botulism, symptoms generally begin 18 to 36 hours after eating contaminated food. However, they can occur as soon as six hours or up to 10 days later. Symptoms may include double or blurred vision, drooping eyelids, slurred speech, difficulty swallowing or breathing, paralysis, a thick-feeling tongue, dry mouth, and muscle weakness.
Trichinella situation
The Argentinian Ministry of Health has also shared updated data on Trichinella in the province of Buenos Aires.
So far in 2023, 160 suspected trichinosis (or trichinellosis) cases have been recorded, this includes 38 confirmed, 56 probable cases and another 65 still under investigation. Three outbreaks have been noted in Chivilcoy, Coronel Dorrego and one that affected several areas.
For the same period in 2022, 210 suspected cases were reported, of which 59 cases were confirmed and 141 were potential infections. Seven outbreaks were recorded.
Trichinellosis is transmitted by eating raw or undercooked pork contaminated with the parasite Trichinella.
Initial symptoms of infection are nausea, diarrhea, vomiting, fatigue, fever, and abdominal discomfort. Headaches, fevers, chills, cough, swelling of the face and eyes, aching joints and muscle pains, itchy skin, diarrhea or constipation may follow. Patients may have difficulty coordinating movements, and have heart and breathing problems.
Abdominal symptoms can occur one to two days after infection. Further symptoms usually start two to eight weeks after eating contaminated meat. Freezing, curing or salting, drying, smoking, or microwaving meat may not kill the organism. The best way to prevent trichinosis is to cook meat to a temperature of 71 degrees C (160 degrees F).
(To sign up for a free subscription to Food Safety News, click here.)
]]>Victory Trading Company Inc.
Greenland, NH
A food firm in New Hampshire is on notice from the FDA for serious violations of the Current Good Manufacturing Practice, Hazard Analysis, and Risk-Based Preventive Controls for Human Food regulation. These violations include the presence of pests in their warehouse.
In an April 17, 2023, warning letter, the FDA described a Dec. 12, 2022, to Jan. 13, 2023 inspection of Victory Trading Company’s ambient, refrigerated and frozen food warehouse in Greenland, NH.
The FDA’s inspection revealed that the firm was not in compliance with regulations and resulted in the issuance of an FDA Form 483. Some of the significant violations are as follows:
Current Good Manufacturing Practice:
1. The firm did not take effective measures to exclude pests from their holding areas and to protect against the contamination of food on the premises by pests. Specifically, rodent activity was observed throughout their warehouse facility including the following:
Rodent Activity Observed
(Redacted)
- On Dec. 12, 2022, during a bag-by-bag examination of (redacted) pallets of (redacted) White Rice, lot # “(redacted)”, stored in the (redacted) corner of their warehouse, apparent rodent excreta pellets (REPs) too numerous to count (TNTC), apparent rodent gnaw holes in the bags of rice, and yellow stains on the bags of rice which smelled like urine and fluoresced UV light. An additional (redacted) pallets of (redacted) White Rice had an odor of urine and apparent REPs.
- On Dec. 13, 2022, an apparent decomposed dead rodent in the (redacted) corner of the warehouse outside the big cooler.
- On Dec. 19, 2022, an apparent decomposed dead rodent in the (redacted) corner of the warehouse outside the freezer.
- On Dec. 15, 2022, apparent REPs TNTC on an empty pallet in pallet location (redacted) in the center of the (redacted) area of the warehouse.
- On Dec. 15, 2022, approximately 10 apparent REPs on the floor below a pallet of bagged dried chili peppers among apparent rodent gnawed material in pallet location (redacted) in the center of the (redacted) area of the warehouse.
- On Dec. 15, 2022, apparent REPs TNTC on the floor behind a pallet of dried noodles in pallet location (redacted) in the center of the (redacted) area of the warehouse.
- On Dec. 15, 2022, approximately 15 apparent REPs on a pallet of BBQ sauce, and apparent rodent urine stains and apparent nesting materials on the floor directly next to pallet in pallet location (redacted) in the center of the (redacted) side of the warehouse.
- On Dec. 15, 2022, approximately 6 apparent REPs on a pallet of plastic cups in pallet location (redacted) in the center of the (redacted) side of the warehouse. The pallet also appeared to contain apparent rodent urine stains, and boxes of cups appeared to have bird excreta on them.
- On Dec. 15, 2022, approximately 13 apparent REPs on the floor in pallet location (redacted) in the center of the (redacted) side of the warehouse.
(Redacted)
- On Dec. 14, 2022, two apparent dead rodents in a glue trap in the (redacted) corner of the warehouse.
- On Dec. 14, 2022, an apparent dead rodent in a glue trap along the (redacted) wall of the warehouse under racks of bags of powdered drink mixes and seeds in pallet location (redacted).
- On Dec. 14, 2022, an apparent dead rodent in a glue trap in the (redacted) corner of the warehouse underneath racks of bagged powdered drink mixes in pallet location (redacted).
- On Dec. 14, 2022, apparent REPs TNTC on the floor at the corner junction of the (redacted) wall of the (redacted) area of the warehouse directly next to pallet location (redacted).
- On Dec. 14, 2022, apparent REPs TNTC on the floor along the (redacted) wall of the (redacted) corner of the warehouse in pallet location (redacted).
- On Dec. 14, 2022, apparent REPs on the floor along the (redacted) wall of the (redacted) corner of the warehouse in pallet location (redacted).
(Redacted)
- On Dec. 15, 2022, an apparent decomposed dead rodent on the floor along the (redacted) wall of the warehouse where bagged rice was stored.
- On Dec. 15, 2022, apparent REPs TNTC on the floor and support beams along the back (redacted) wall where bagged rice was being stored.
- On Dec. 13, 2022, apparent REPs TNTC and apparent nesting material observed in the (redacted) section of the warehouse on the floor touching and directly next to pallets of (redacted) White Rice.
- On Dec. 14, 2022, apparent REPs on the floor in the (redacted) area of the warehouse (next to the employee bathroom) in pallet location (redacted).
- On Dec. 14, 2022, apparent REPs and apparent rodent urine stains which fluoresced under UV light along the (redacted) wall of the (redacted) area of the warehouse in pallet location (redacted).
- On Dec. 14, 2022, apparent REPs on the floor in the (redacted) corner of the (redacted) area of warehouse in pallet location (redacted).
- On Dec. 14, 2022, approximately 6 REPs on the floor directly next to a pallet of rice sticks in pallet location (redacted) in racks along the (redacted) wall of the (redacted) side of the warehouse.
- On Dec. 14, 2022, approximately 20 apparent REPs on a pallet of vinegar in pallet location (redacted) in racks along the (redacted) wall of the (redacted) side of the warehouse.
- On Dec. 14, 2022, approximately 5 apparent REPs on the floor approximately 6” from a pallet of maltose in pallet location (redacted) in racks along the (redacted) wall of the (redacted) side of the warehouse.
- On Dec. 14, 2022, apparent REPs TNTC on a pallet which contained jasmine tea in pallet location (redacted) in storage racks along the (redacted) wall in the (redacted) side of the warehouse.
- On Dec. 15, 2022, apparent REPs TNTC on a pallet of plastic take-out containers in pallet location (redacted) in storage racks along the (redacted) wall in the (redacted) side of the warehouse.
- On Dec. 14, 2022, approximately 20 apparent REPs on the floor scattered directly next to a pallet of dried seaweed in pallet location (redacted) in storage racks along the (redacted) wall in the (redacted) side of the warehouse.
- On Dec. 14, 2022, a live insect and apparent REPs TNTC on a pallet of dried spices in pallet location (redacted) in storage racks along the (redacted) wall in the (redacted) side of the warehouse.
- On Dec. 14, 2022, approximately 8 apparent REPs on a pallet of rice sticks in pallet location (redacted) in storage racks along the (redacted) wall in the (redacted) side of the warehouse.
(Redacted)
- On Dec. 18, 2022, apparent REPs TNTC on the floor and on support beams along the (redacted) wall behind coolers (redacted) and (redacted).
- On Dec. 19, 2022, approximately 10 apparent REPs on a table holding shrink wrap stored along the (redacted) wall.
- On Dec. 19, 2022, approximately 15 REPs along the (redacted) wall upstairs in the equipment storage room (redacted) main office. Additionally, the rodent station (redacted) was missing from its designated wall location.
- On Dec. 19, 2022, approximately 14 apparent REPs at the top corner of the stairs leading to the equipment storage room (redacted) main office located at the (redacted) wall of the warehouse.
- On Dec. 19, 2022, approximately 25 apparent REPs in the (redacted) corner of the equipment storage room (redacted) main office located at the (redacted) wall of the warehouse.
- On Dec. 19, 2022, approximately 15 apparent REPs along the (redacted) wall of the equipment storage room (redacted) main office located at the (redacted) wall of the warehouse.
- On Dec. 14, 2022, apparent REPs TNTC on the floor at the corner junction of the (redacted) wall and the big cooler in the (redacted) side of the warehouse where bagged sugar was being stored.
- On Dec. 19, 2022, approximately 2 apparent REPs on the floor in the walk-in freezer closest to the big cooler along the (redacted) wall in the (redacted) area of the warehouse.
- On Dec. 14, 2022, apparent REPs TNTC on the floor in the center aisle of the warehouse in pallet location (redacted) of the (redacted) area of the warehouse.
- On Dec. 14, 2022, approximately 11 apparent REPs on a pallet of (redacted) noodles and approximately 15 REPS in a center food storage rack in the (redacted) side of the warehouse in pallet location (redacted).
- On Dec. 13, 2022, apparent REPs TNTC on a rack in pallet location (redacted) and (redacted) of the central aisle storage racks in the (redacted) area of the warehouse used to hold (redacted) Brown Rice in paper bags and (redacted) Potato Starch in paper bags. Additionally, apparent rodent paw prints and tail marks were observed in spilled product on the racks.
- On Dec. 14, 2022, approximately 10 apparent REPs on the floor behind a pallet of bagged rice in pallet location (redacted) of the central aisle storage racks in the (redacted) area of the warehouse.
- On Dec. 14, 2022, apparent REPs on the floor along the (redacted) wall of the (redacted) area of the warehouse in pallet location (redacted) directly below and next to bags of palleted rice.
- On Dec. 14, 2022, apparent REPs TNTC were observed on the floor along the (redacted) wall and under a food storage rack on the left-hand sides of cooler (redacted) in the (redacted) area of the warehouse.
Samples
FDA collected several samples during the inspection. These samples included a food product sample ((redacted) White Rice) and filth samples. These samples were submitted to FDA labs for analysis. Results demonstrate that the (redacted) White Rice and sample 1209823 were contaminated with rodent excreta pellets (REPs), and sample 1209822 was contaminated with rodent excreta pellets and rodent nesting material. The filth samples further demonstrate the presence of rodents throughout the facility.
2. The firm did not maintain their plant in a clean and sanitary condition and keep their plant in repair adequate to prevent food from becoming adulterated. Specifically, insanitary conditions were observed throughout their facility demonstrating that sanitation, cleaning, and maintenance operations were inadequate. The following observations reflect potential areas for pest harborage and attractants for pests:
(Redacted)
- On Dec. 13, 2022, a 24″ x 8″ rip in the insulation liner of the (redacted) wall exposing insulation. The exposed insulation had been partially removed and apparent REPs TNTC were observed inside the insulation.
- On Dec. 13, 2022, an approximate 1/4″ hole through the wall to the outside and an approximate 12″ x 12″ rip in the insulation liner of the (redacted) wall. An empty beer bottle was observed in the hole.
- On Dec. 15, 2022, an approximate 2-3” gap along the entire length of the (redacted) wall creating a potential ingress for pests.
- On Dec. 15, 2022, an approximate 1” wide crack in the floor approximately 12” from pallet location (redacted) creating a potential ingress for pests near the (redacted) wall in the warehouse.
- On Dec. 15, 2022, an approximate ½” gap in the floor approximately 6” from pallet location (redacted) in the (redacted) area of the warehouse. There appeared to be hollow space beneath the gap.
(Redacted)
- On Dec. 13, 2022, two overhead doors on the (redacted) side of the warehouse occupied by a moving and storage company were left open for an extended period during the day creating a potential ingress for pests.
(Redacted)
- On Dec. 13, 2022, spilled unknown white powder product on a pallet of soybean oil stored in the (redacted) section of the warehouse.
- On Dec. 15, 2022, an approximate 1” gap closest to the (redacted) wall of the warehouse creating a potential ingress for pests. The area below the gap appeared to be hollow.
- On Dec. 13, 2022, two approximate 1” gaps around electrical conduits in the (redacted) wall of the warehouse creating an opening to the outside.
(Redacted)
- On Dec. 12, 2022, the plastic liner of the dividing wall in the center of the warehouse in the (redacted) side contained what appeared to be rodent gnaw holes and apparent REPs inside the insulation in the wall. Apparent rodent nesting materials were observed on the ground, and gnaw marks were observed on a wooden post of the dividing wall.
- On Dec. 14, 2022, red onions in a bag made of plastic netting stored directly on the floor within 6” from where apparent REPs were observed outside the main office in the (redacted) side of the warehouse.
- On Dec. 14, 2022, stagnant clear liquid on the floor of coolers (redacted) and (redacted) creating a potential attractant for pests and a potential harborage area for bacteria in the (redacted) area of the warehouse.
- On Dec. 19, 2022, what appeared to be apparent rodent-gnawed material, apparent REPs TNTC, and insulation used as apparent rodent nesting material in the equipment storage trailer that is permanently affixed to the outside of the (redacted) wall.
3. The firm did not maintain their facility’s grounds in a condition adequate to protect food from becoming contaminated. Specifically, on Dec. 14, 2022, an overgrowth of weeds and vegetation were observed outside on the eastern and northern sides of the warehouse, creating potential harborage areas for pests.
The full warning letter can be viewed here.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The webinar, titled “Facing Food Safety Challenges through Culture and Persistence,” will feature distinguished guest speakers, including Kerry Bridges, Vice President of Food Safety at Chipotle Mexican Grill; Al Almanza, Global Head of Food Safety and Quality Assurance at JBS Foods; Lone Jespersen, Principal and Founder of Cultivate SA; and Conrad Choiniere, Director of the Office of Analytics and Outreach at the Center for Food Safety and Applied Nutrition, FDA.
This collaborative series brings together experts from both the public and private sectors to exchange ideas and experiences regarding the importance of cultivating a robust food safety culture, ultimately contributing to safer food production.
According to the FDA, food safety culture stands as a cornerstone in the FDA’s New Era of Smarter Food Safety blueprint. This strategic blueprint emphasizes the need to influence the beliefs, attitudes and behaviors of individuals and organizations to achieve significant reductions in foodborne illnesses.
For those interested in participating in this enlightening webinar, you can register here.
To access additional information about the webinar series and to listen to past sessions, visit “Collaborating on Culture in the New Era of Smarter Food Safety.”
About STOP
STOP Foodborne Illness, a dedicated public health non-profit organization, has been advocating for food safety since 1994. With a mission to educate and inform the public about the importance of food safety through personal advocate stories, STOP Foodborne Illness is a dedicated team working to prevent foodborne illnesses and fatalities. More information can be found on their website, stopfoodborneillness.com
(To sign up for a free subscription to Food Safety News, click here.)
]]>Cooling and packing food
One common oversight is improper cooling of freshly cooked food. Failing to cool cooked dishes promptly can lead to rapid bacterial growth. After cooking, it’s crucial to cool food quickly and store it in shallow containers for immediate refrigeration or transportation.
Washing fruits and vegetables
Washing fruits and vegetables before cutting is essential to prevent the transfer of bacteria from the peel or rind to the flesh. After washing, store cut produce in waterproof containers or plastic wrap to ensure it cools properly before being placed in picnic coolers.
Cooler location
To maintain food safety, the placement of coolers is vital. It’s advisable to keep coolers in the passenger area of a vehicle instead of the trunk, where temperatures tend to be higher. Once at the picnic site, place the cooler in the shade and cover it with a blanket, keeping it closed until it’s time to eat.
Keep cold foods cold, hot foods hot
Cold foods should remain cold, while hot foods must stay hot to prevent bacteria and pathogens from multiplying. Ice packs and frozen gel packs are essential additions to coolers, and insulated containers with boiling water can keep foods hot until serving.
Handling food and handwashing

Thorough handwashing is crucial when handling food, especially as multiple hands are involved in preparing and serving dishes. In the absence of running water, hand sanitizers and paper towels can be used, though they are not as effective. Utensils and dishes should be plentiful to prevent cross-contamination, especially when preparing meats like poultry, fish, and beef.
Proper grilling
Grilling is a popular Labor Day activity, but it also poses food safety challenges. The USDA recommends three key steps for safe grilling:
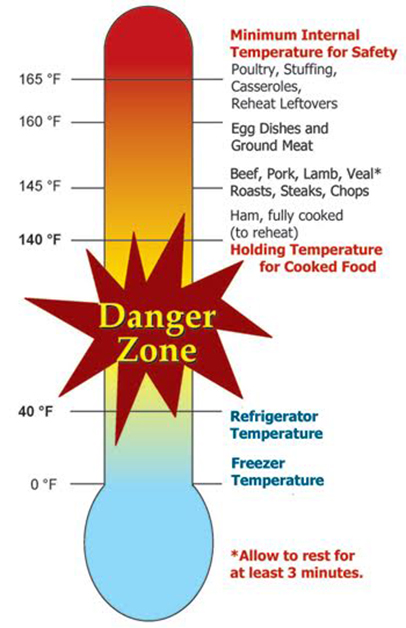
- Place the Thermometer: Insert a thermometer into the thickest part of the meat to check its internal temperature.
- Read the Temperature: Wait for an accurate reading, following USDA guidelines for safe temperatures.
- Off the Grill: Remove meat and poultry from the grill once they reach their safe minimum internal temperatures, avoiding contact with raw meat or poultry.
Handling Leftovers To ensure food safety with leftovers, remember the two-hour rule: perishable items should be refrigerated within two hours (or one hour in temperatures above 90°F) to prevent bacterial growth. Use small, shallow containers for quicker cooling and freeze or consume leftovers within four days.
Reheating When reheating, cover and rotate food for even heating, especially in the microwave. Reheat sauces, soups, and gravies to a rolling boil. Slow cookers should not be used for reheating. Leftovers are safe to eat when they reach an internal temperature of 165°F.
Traveling food safety tips
For those hitting the road this Labor Day, the USDA offers the following tips to ensure food safety while traveling:
- Pack perishable foods directly from the refrigerator or freezer into the cooler.
- Use an appliance thermometer in the cooler to maintain temperatures at or below 40°F.
- Keep raw meats and poultry separate from cooked or raw foods meant to be consumed without further cooking.
- Consider using two coolers for immediate needs and perishable items.
- Choose bottled or canned drinks when camping, as untreated water from streams and rivers can be unsafe.
- Prioritize hand hygiene with hand sanitizers containing at least 60 percent alcohol.
- Think about purchasing shelf-stable food options to guarantee food safety on the go.
- While at the beach, partially bury the cooler in the sand, cover it with blankets, and use a beach umbrella for shade.
- Avoid consuming food that has been sitting out for more than two hours (or one hour in temperatures above 90°F).
By following these food safety guidelines, Americans can ensure a healthy and enjoyable Labor Day celebration, free from the risks of foodborne illnesses.
For additional food safety inquiries, individuals can contact the USDA Meat and Poultry Hotline at 888-MPHotline (888-674-6854) or chat live at ask.usda.gov from 10 a.m. to 6 p.m. EDT Monday through Friday.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The majority of topics highlighted at a recent World Trade Organization (WTO) meeting on food safety had already been discussed before.
At the WTO Committee on Sanitary and Phytosanitary (SPS) Measures meeting in July, members addressed specific trade concerns relating to food safety and animal and plant health.
A total of 46 trade concerns were discussed — one new and 45 previously raised — covering issues such as pesticide residues, import restrictions due to BSE, COVID-19 related suspensions, delays in approval procedures, cadmium in chocolate and cocoa, and animal health-related restrictions.The one new area was Canada’s restrictions on Brazilian pork from internationally recognized foot and mouth free zones without vaccination.
Ukraine shared information on the current functioning of its SPS infrastructure and other aspects of the food security situation. Russian officials said discussions about the war were outside the scope of the WTO.
U.S concern over Chinese rules
The United States repeated that it remains “deeply concerned” with China’s lack of explanation on how two decrees address food safety and public health. The United States said China has not provided the scientific basis or risk assessment that informed their development.
The United States added that new registration requirements that came into effect after June 30, 2023 have caused “significant” confusion for exporters due to the lack of clear guidance. This issue has been ongoing since 2020 and other nations to express concern about the plans include Japan, the European Union, the United Kingdom, Australia, and Canada.The European Union gave information on proposals around plants obtained by certain new genomic techniques and their food and feed, which sets out rules for the use of such plants as part of EU sustainability initiatives. The EU also reported on recommendations to combat antimicrobial resistance as part of the One Health approach.
Japan provided an update on the Fukushima nuclear power station accident emphasizing that monitoring data shows the level of radioactivity is very low and Japanese food is safe for the public. In late August, Japan started releasing treated water from the site into the sea. China has suspended imports of seafood from Japan and Hong Kong banned aquatic products from 10 areas in Japan, including all live, frozen, chilled, dried or otherwise preserved aquatic products, sea salt, and unprocessed or processed seaweed.Australian officials said they had confidence in the process that led to the decision to release the treated water and the move was also supported by the United States and United Kingdom.
The next meeting of the SPS Committee is scheduled for mid-November 2023.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The frozen chicken strips entrees were produced on June 20, 2023, July 11, 2023, and July 17, 2023. The following products subject to recall are:
- 8.9-oz. carton containing one entree of “BANQUET CHICKEN STRIPS MEAL” with best if used by “DEC 11 2024,” “JAN 01 2025,” or “JAN 07 2025” and lot numbers 5009317120, 5009319220, or 5009319820 located on the side of the carton
The products subject to recall bear the establishment number “EST. P-9” printed on the side of the carton. These items were shipped to retail locations nationwide and were also sold online.
The mistake was discovered when the firm notified FSIS that it received a consumer complaint of plastic in the chicken strip portion of the product, resulting in an oral injury associated with consuming it.
FSIS has not yet received additional reports of injury or illness from consumption of these products. Anyone concerned about an injury or illness should contact a healthcare provider.
FSIS is concerned that some products may be in consumers’ freezers. Consumers who have purchased these products are urged not to consume them. These products should be thrown away or returned to the place of purchase.
FSIS routinely conducts recall effectiveness checks to verify that recalling firms notify their customers of the recall and that steps are taken to ensure that the product is no longer available to consumers. The retail distribution list(s) will be posted on the FSIS website when available.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The ready-to-eat blended meat and poultry smoked sausage items were produced on June 14, 2023. The following products are subject to the recall:
- 14-oz. Package containing one rope of “HILLSHIRE FARM SMOKED SAUSAGE MADE WITH PORK, TURKEY, BEEF” with lot codes in the form of the establishment number, line number and time of production in hours:minutes: seconds, “EST. 756A 20 19:00:00 through 21:59:59 and EST. 756A 21 19:00:00 through 21:59:59” and use by date of “Nov 11 23” printed on the front of the package.
The products subject to recall bear the establishment number “EST. 756A” printed on the front of the package. These items were shipped to California, Maryland, New Mexico, New York, North Carolina, Pennsylvania, and Virginia retail stores.
The problem was discovered when the firm notified FSIS that it received consumer complaints regarding bone fragments in the product. Also, FSIS received one consumer complaint regarding this issue.
There has been one reported oral injury associated with the consumption of this product. FSIS has received no additional reports of injury or illness from consumption of these products. Anyone concerned about an injury or illness should contact a healthcare provider.
FSIS is concerned that some products may be in consumers’ refrigerators or freezers. Consumers who have purchased these products are urged not to consume them. These products should be thrown away or returned to the place of purchase.
FSIS routinely conducts recall effectiveness checks to verify that recalling firms notify their customers of the recall and that steps are taken to ensure that the product is no longer available to consumers. The retail distribution list(s) will be posted on the FSIS website when available.
(To sign up for a free subscription to Food Safety News, click here.)
]]>A total of 33 confirmed and one probable case were linked to a pub in Wrexham.
Despite an investigation and testing, the precise source or route of transmission in the Salmonella Infantis outbreak was not identified.
In late July, an Outbreak Control Team (OCT) was established including Public Health Wales, Betsi Cadwaladr University Health Board and Wrexham County Borough Council’s environmental health team.
No details on the age range or gender of patients were released to protect their identity.
Source of outbreak unknown
Richard Firth, consultant in public health at Public Health Wales, and chair of the OCT, said several cases of Salmonella were identified in Wrexham at the end of July.
“We can confirm a total of 33 confirmed, genomically identical, cases of Salmonella infection and one probable case associated with The Nags Head public house on Mount Street, Wrexham, owned by Marston’s PLC,” he said.
“On July 31, control measures were put in place, which included a voluntary closure and deep clean of the premises, and testing of all staff. No further cases have been identified since the control measures were put in place.
“Whilst all the evidence indicates the exposure site for the infections being The Nags Head, extensive investigation and testing has not identified the precise source or route of transmission for the infections. Public Health Wales would like to extend our sympathies to those affected by this outbreak. We would also like to thank our multi-agency partners as well as the management and staff at both The Nags Head and Marston’s PLC for their proactive support throughout this investigation.”
About Salmonella
Food contaminated with Salmonella bacteria does not usually look, smell, or taste spoiled. Anyone can become sick with a Salmonella infection. Infants, children, seniors, and people with weakened immune systems are at higher risk of serious illness because their immune systems are fragile, according to the CDC.
Anyone who has developed symptoms of Salmonella food poisoning should seek medical attention. Sick people should tell their doctors about the possible exposure to Salmonella bacteria because special tests are necessary to diagnose salmonellosis. Salmonella infection symptoms can mimic other illnesses, frequently leading to misdiagnosis.
Symptoms of Salmonella infection can include diarrhea, abdominal cramps, and fever within 12 to 72 hours after eating contaminated food. Otherwise, healthy adults are usually sick for four to seven days. In some cases, however, diarrhea may be so severe that patients require hospitalization.
Older adults, children, pregnant women, and people with weakened immune systems, such as cancer patients, are more likely to develop a severe illness and serious, sometimes life-threatening conditions. Some people get infected without getting sick or showing any symptoms. However, they may still spread the infections to others.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The Minnesota Department of Health urges anyone who recently purchased milk from Healthy Harvest Farm and Kitchen to discard the product and not consume it. The milk may be labeled natural A2 milk, and consumers may be unaware that the milk has not been pasteurized.
The illnesses have been caused by Cryptosporidium parvum, a parasite commonly found in cattle. The cases have related subtypes of Cryptosporidium parvum, suggesting a common source.
All people who became ill with gastrointestinal symptoms in early August reported purchasing or consuming raw milk from Healthy Harvest Farm and Kitchen before the onset of their illness. Four of them are younger than 10, and one has been hospitalized. One person was infected with Cryptosporidium parvum and E. coli O111:H8 at the same time. Being infected with multiple germs is not uncommon in raw milk outbreaks.
Raw or “natural” milk has not gone through the pasteurization process that heats the milk to a high temperature for a short period of time to kill harmful fecal germs that can contaminate raw milk. These germs can include Cryptosporidium, E. coli, Salmonella, and other viruses, bacteria and parasites, leading to the possibility of getting multiple infections from raw milk. Pasteurization is the only effective method for eliminating germs in raw milk and does not significantly change milk’s nutritional value.
“Cattle can naturally carry Cryptosporidium and E. coli in their digestive system and shed these germs in their manure even though the animal is not sick. Contamination of the milk with manure can occur during the milking process, and if the milk is not pasteurized, the germs will not be killed,” said Carrie Klumb, senior epidemiologist in the Zoonotic Diseases Unit at MDH. “Consuming any unpasteurized milk, no matter how well the animals are cared for and how clean the operation is, puts people at risk for getting sick.”
People infected with Cryptosporidium generally develop watery diarrhea, stomach cramps, loss of appetite, and weight loss approximately a week after consuming contaminated foods or touching infected animals. The illness typically lasts two weeks, but symptoms may go in cycles in which people seem to get better for a few days and then feel worse again before the illness ends.
Symptoms of E. coli infections typically include stomach cramps and diarrhea, including bloody diarrhea. People typically become ill two to five days after consuming contaminated food. In some cases, people may develop severe illness that leads to hospitalization.
Children under the age of 5, adults over 65, and those with weakened immune systems are most at risk.
The health department is working to identify all people who may have purchased milk from Healthy Harvest Farm and Kitchen to inform them of the risks to prevent additional illnesses. If you or someone you know has experienced gastrointestinal illness after consuming unpasteurized milk from Healthy Harvest Farm and Kitchen, please complete a confidential online survey or email [email protected]. If you are sick, please get in touch with your healthcare provider.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Earlier this week, the Centre for Health Protection (CHP) of the Department of Health revealed a suspected puffer fish poisoning case and reminded people not to consume puffer fish.
The patient is an 84-year-old man who developed dizziness, finger numbness and shortness of breath about one hour after eating cooked puffer fish, which was caught by himself on the same day in local waters. He was admitted to a hospital for treatment and is in stable condition.
Certain organs of puffer fish have high concentrations of tetrodotoxin, which is a potent neurotoxin that can affect the central nervous system. The toxin is not removed by cooking, boiling, drying or freezing.
In another incident, suspected neurotoxic shellfish poisoning affected two people.
A 42-year-old female and a 45-year-old male presented with tingling of the tongue, vomiting and diarrhea a few minutes to three hours after consuming steamed snails at home. An initial investigation revealed the snails were bought from a seafood stall at Ap Lei Chau Market.
“Neurotoxic shellfish poisoning toxin is a natural toxin sometimes found in bivalve shellfish. It is heat-stable and cannot be destroyed through cooking,” said a CHP spokesman.
Advice from officials included sourcing shellfish from places where monitoring programs for toxins have been established and to only purchase such products from reliable sources.
Bacterial outbreaks
CHP also investigated two suspected food poisoning clusters affecting five people.
The first cluster had two females, aged 29 and 30, who developed abdominal pain, diarrhea, nausea, vomiting and fever about 15 hours after eating at a restaurant in Tsim Sha Tsui. The other cluster involved three females, aged 22 to 49, who had similar symptoms about 14 hours after having dinner at this restaurant on the same day. Two people were hospitalized.
Initial investigations pointed to pancakes made with eggs as the source of illness that might have been caused by Salmonella.
An imported case of Shiga toxin-producing E. coli (STEC) infection was recorded in mid-August.
A 2-year-old boy was suffering from vomiting in early August, and then had a fever, abdominal pain and diarrhea the next day. He was taken to hospital and admitted before being discharged the next day after his condition became stable. STEC was detected in a stool specimen.
The patient had been to Malaysia from July 29 to August 3. He had consumed yogurt and fresh fruit juice, and had contact with animals. He also swam at the beach and in a swimming pool. Two family members also recorded similar symptoms but had recovered.
The largest outbreak sickened at least 55 people. It involved 24 males and 31 females, aged 7 to 49, who came down with abdominal pain and diarrhea eight to 16 hours after having dinner at a canteen of a campsite in Tai Po.
Officials suspected penne carbonara contaminated with Clostridium perfringens as the source of illness. Initial investigations revealed a possible reason for the incident was improper food holding temperatures.
Wild plants and bamboo shoot
In mid-August, a 69-year-old woman fell sick after accidentally consuming part of a dangerous plant. CHP reminded the public not to pick or consume wild plants, and to be aware of vegetables containing calcium oxalate raphide.
The patient reported oral numbness, a burning sensation of the mouth and shortness of breath shortly after consuming a wild taro that she was given as a gift from a friend in Tai Po.
Taro is a popular ingredient used to prepare various dishes and desserts. However, some plants look like taro, such as giant alocasia, but contain toxins that can cause food poisoning.
CHP has also advised people not to consume raw bamboo shoot after a 67-year-old man and a 50-year-old woman fell ill.
The male patient bought fresh bamboo shoots from a shop in Mei Foo and the female patient pressed them into juice at home on the same day. The duo developed headache, dizziness, palpitation, nausea, limb numbness and shortness of breath 10 minutes after drinking the juice.
“Raw bamboo shoot contain cyanogenic glycosides. Cyanogenic plant products such as bamboo shoot can cause poisoning when eaten raw and in sufficient amounts. Cyanogenic plants should be cut into smaller pieces, soaked in water and cooked thoroughly in boiling water before consumption,” said a CHP spokesman.
(To sign up for a free subscription to Food Safety News, click here.)
]]>All parts of the yellow oleander plant are known to contain cardiac glycosides that are highly toxic to humans and animals. Ingestion of yellow oleander can cause neurologic, gastrointestinal, and cardiovascular adverse health effects that may be severe, or even fatal. Symptoms may include nausea, vomiting, dizziness, diarrhea, abdominal pain, cardiac changes, dysrhythmia, and more.
The product was distributed online through the Amazon, eBay, and Walmart platforms. The product comes in a 2-ounce white with green marked foil bag. 12 seeds in a bag.
No illnesses have been reported to date.
The recall was the result of sampling conducted by the FDA.
Consumers who purchased Nuez de la India seeds from Todorganic Inc. are urged to return it to the place of purchase for a full refund. Consumers with questions can contact the company at 904-397-9339 Carlos Perez.
(To sign up for a free subscription to Food Safety News,click here)
]]>According to the details posted online by the FDA, the recall was initiated on Aug. 15, 2023, and is ongoing.
The recalled products were sold in California, Connecticut, Florida, Illinois, Pennsylvania, Texas and Washington.
Recalled products:
- Trader Joe’s Multigrain Crackers with Sunflower and Flax Seeds
- 10oz (283g) box
- UPC 000000761567
- 24 retail boxes per wholesale case
- Product Quantity: 13,132 cases
- Code Information: Lot Code – 1GF06053, BEST IF Used By Date – 03 01 24; Lot Code – 1GF06063, BEST IF Used By Date – 03 02 24; Lot Code – 1GF06073, BEST IF Used By Date – 03 03 24; Lot Code – 1GF06083, BEST IF Used By Date – 03 04 24; Lot Code – 1GF06093, BEST IF Used By Date – 03 05 24
Anyone who purchased the recalled products should immediately dispose of it and not consume it.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Hurricane Idalia looms over florida
As Hurricane Idalia intensified moves through Florida and up the U.S. coast, residents are on high alert.
Tropical Storm Idalia rapidly transformed into a Category 3 hurricane. Life-threatening storm surges and dangerous winds have swept through various parts of Florida and forecasters predict it will continue up the coast.
West Virginia suffers from unrelenting flooding
As Florida prepared for Hurricane Idalia, West Virginia grappled with the aftermath of excessive rainfall, leading to widespread flooding. Gov. Jim Justice declared a State of Emergency for Kanawha, Braxton, Calhoun, Clay, and Roane counties. The torrential rains have inflicted damage upon homes, bridges, and roads in these regions.
Gov. Justice’s statement can be found here.
Ensuring food safety amidst the chaos
With both regions facing unique challenges, ensuring food safety during and after these catastrophic events remains a top priority. The U.S. Food and Drug Administration and other organizations provide crucial guidelines for residents to safeguard their food and health.
Before a storm hits:
- Elevate refrigerators and freezers off the ground using cement blocks.
- Move canned goods and foods from basements or low cabinets to higher areas.
Food safety after flooding:
- Use bottled drinking water that hasn’t come into contact with floodwater.
- Discard any food that may have been exposed to floodwater, particularly if not in waterproof containers.
- Inspect canned foods for damage, and discard damaged cans.
- Thoroughly wash and sanitize metal pans, dishes, and utensils using a chlorine bleach solution.
During power outages:
- Keep refrigerator and freezer doors closed to maintain safe temperatures.
- Use ice packs, coolers, and frozen containers of water or gel packs to preserve food freshness.
After power restoration:
- Check refrigerator and freezer temperatures; follow guidelines for safe food storage.
- Discard perishable foods that have been at temperatures above 40 degrees F for 4 hours or more.
- Refreeze frozen food if temperature remains at 40 degrees F or below.
Farmers’ concerns and resources:
- For farmers, these weather events pose serious risks to their crops. The FDA provides guidance on assessing potential damage to food crops affected by floods. If edible portions of crops are exposed to contaminated floodwaters, they’re considered adulterated and unsuitable for human consumption. Farmers are advised to evaluate the safety of crops on a case-by-case basis for potential food safety concerns.
Both West Virginia and Florida are currently marshaling resources, emergency teams, and relief efforts to aid affected residents. By following these essential food safety tips, individuals can better protect themselves and their families during these trying times. For more information, residents can access resources provided by local health departments and relevant agencies, or contact the USDA Meat and Poultry Hotline at 888-MPHotline.
Stay safe, stay informed, and stay prepared as these natural disasters unfold.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Reports in early August suggested post-Brexit border controls were to be pushed back for the fifth time.
Sanitary and phytosanitary controls were delayed for three months and will now be introduced beginning Jan. 31, 2024. This includes health certification on imports of medium risk animal products, plants, plant products and high risk food and feed of non-animal origin from the EU.
Documentary and risk-based physical inspections on medium risk animal products, plant products and high risk food and feed of non-animal origin from the EU will be implemented in late April 2024.
The Border Target Operating Model was developed with the help of the Scottish and Welsh Governments and following engagement with businesses in the UK.
Phytosanitary certificates will be digitized from 2023 with take-up depending on the readiness of trade partners.
Officials said risks from inadequate controls were significant. A recent UK-wide Salmonella outbreak caused by chicken products from Poland resulted in more than 1,000 confirmed illnesses, with potentially as many as 4,000 additional cases that were not reported, and cost an estimated £7.7 million ($9.7 million).
Recent inspections of shops by local authorities in the UK detected frozen, raw and uncooked meat products marked as suitable only for sale in the originating country. Further investigations found the items had been purchased by two importers, linked to more than 280 UK retail outlets. Products were exported commercially and pre-notified on the UK imports system. Although they didn’t test positive for African Swine Fever, the fact they reached the UK presents a serious threat to the pig industry.
Reaction to model and new timelines
Nigel Jenney, CEO of the Fresh Produce Consortium, said: “It’s clear, government has acted upon our concerns and will now implement a unique border approach for the benefit of consumers and industry. This focused risk-based approach will reinforce UK biosecurity and promote self-regulation to minimize supply chain disruption.”
The Chartered Institute of Environmental Health (CIEH) said there remains ambiguity about the future charging mechanism for checks. The group said fees and charges should be set at the local level to account for the unique requirements and resources of individual regions.
CIEH added there was a need for clarity in the risk categorization of goods. The distinction between high, medium, and low-risk is vital to ensure that controls maintain high standards without causing unnecessary delays.
“While the Border Target Operating Model promises an efficient and effective system, CIEH and our members have been consistent in demanding that it remains robust in safeguarding public health, food safety, and biosecurity. Furthermore, while we wholeheartedly support innovations that streamline trade and enhance security, it’s essential that such schemes are not introduced at the expense of rigorous safety and public health controls,” said Louise Hosking, executive director of environmental health.
Nichola Mallon, head of Trade and Devolved Policy at Logistics UK, said the group will study the model to see if it provides the detail needed by members and EU suppliers.
“Will three months be sufficient time for government to provide the necessary technical detail and guidance that businesses will need to change processes and adapt to the changes outlined by the new trading arrangements?,” she asked.
“After so much time, and so many delays, logistics businesses are losing confidence in the government’s ability to provide workable solutions to enable the new trading arrangements to be implemented.”
The National Farmers Union (NFU) said the delay was “hugely frustrating”.
“For the past three years, our farmers have faced the full reach of EU controls on our exports while the EU has enjoyed continued easy access to the UK marketplace. It’s hugely frustrating for many producers that the government has yet again delayed the implementation of vital checks on goods entering from the EU,” said Minette Batters, NFU president.
The International Meat Trade Association (IMTA) raised concerns about the exact rates of physical checks, risk categories for rest of world products and the SPS charging regime.
“I think the delay will come as a relief to many of our members who have been concerned about the introduction of certification for imports from the EU and how that will impact on just in time supply chains. We hope that there will be a redoubling of efforts from government to engage with industry to ensure that when the, now delayed, changes are introduced sufficient consideration is given to just in time supply chains,” said Dan Soper, IMTA policy manager.
(To sign up for a free subscription to Food Safety News, click here.)
]]>By bringing together the science from CDC, FDA and FSIS, and by developing sound analytical methods, IFSAC’s goal was to improve estimates of the sources of foodborne illness.
IFSAC this week announced its priorities for 2024 to 2028
During 2024 – 2028 IFSAC will focus on generating the most accurate and actionable estimates for foodborne illness source attribution in the United States by leveraging the latest science, data, and methods, and will communicate these estimates to stakeholders in government, industry, academia, and consumer organizations.
Here are the four priorities for the 5-year period:
Priority 1: Explore additional data sources and alternative methods to better estimate the sources of foodborne illnesses caused by Campylobacter and harmonize estimates across different approaches and data sources.
IFSAC’s annual Foodborne Illness Source Attribution reports have aimed to estimate food category sources of Campylobacter illnesses using foodborne outbreak data. However, the sources of reported Campylobacter outbreaks differ considerably from the sources of non-outbreak- associated illnesses as reported by other types of epidemiological studies. One major concern is that the food products most frequently associated with Campylobacter outbreaks such as raw milk and chicken livers are rarely consumed. Therefore, outbreak data are not representative of sources of Campylobacter in the general U.S. population. For these reasons, IFSAC paused reporting of attribution estimates for Campylobacter in 2022. IFSAC aims to produce more reliable and generalizable Campylobacter source attribution estimates in the future.
Priority 2: Expand our list of priority pathogens to include non-O157 Shiga toxin-producing E. coli (STEC) and provide source attribution estimates in IFSAC’s annual Foodborne Illness Source Attribution reports.
Non-O157 STEC is an important cause of foodborne illness in the United States and of increasing importance to federal food safety regulatory agencies. IFSAC will leverage existing non-O157 STEC data and analytical methods to estimate source attribution for this pathogen and incorporate these estimates in IFSAC Annual Attribution Reports.
Priority 3: Consider incorporating data on non-foodborne sources of priority pathogens, such as animal and environmental sources, into IFSAC’s annual Foodborne Illness Source Attribution estimates to better refine and contextualize foodborne illness source attribution estimates.
Although the priority pathogens included in IFSAC’s analyses are spread predominantly through food-borne transmission, these pathogens also spread through contact with water, human, animal, and environmental sources. To generate more accurate estimates for food-borne illness source attribution, IFSAC analysts will explore available data for non-foodborne sources of the priority pathogens and consider methods to incorporate this information in communications.
Priority 4: Finalize existing analyses and disseminate findings to multiple audiences. IFSAC is engaged in numerous projects (description of current and completed projects can be found on the IFSAC website), many of which have not been communicated through peer-reviewed journal articles or other publications. To ensure sufficient resources for IFSAC’s priority research areas during 2024 – 2028, IFSAC will review the status of all projects, determine which are close to completion, and identify which should be finalized and by when. During the final stages of each project, IFSAC will pursue and implement appropriate communication vehicles for each project, such as peer-reviewed publications, public reports, webinars, conference presentations, or updates to the IFSAC website to disseminate findings to the appropriate audiences including regulatory agencies, public health partners, academics, media, industry and the public.
Purpose
IFSAC published an initial strategic plan to outline its shared goals and objectives for the first five years of the collaboration, 2012 – 2016, which was followed by a strategic plan for 2017 – 2021 and an interim plan for 2022 – 2023.
These documents outlined a commitment to improving foodborne illness source attribution estimates for the United States by focusing on three general areas: improving and expanding data, improving and expanding analytical methods, and improving and increasing communication activities. A description of projects, associated publications, and presentations are available on the IFSAC website.
Over the next five years, IFSAC intends to continue publishing annual reports with updated estimates of foodborne illness source attribution. IFSAC reiterates its overall focus and outline for priorities that will guide the work during calendar years 2024 – 2028.
(To sign up for a free subscription to Food Safety News, click here.)
]]>The recalled products were sold at the Ice Cream House in Brooklyn, NY, and through retail supermarkets in New York, New Jersey, and Ohio, according to the company’s recall notice posted by the Food and Drug Administration this afternoon.
This recall is related to the soft serve On The Go cups previously recalled by Real Kosher Ice Cream Inc., where two cases of illnesses have been reported in this outbreak in New York and Pennsylvania. Both individuals were hospitalized, but no deaths have been reported to date.
Consumers can use the following information to identify the recalled products:
The company has ceased producing and distributing the products as the investigation is ongoing.
The newly recalled products include all Ice Cream House branded items currently on the market. This includes all dairy and non-dairy (Parve) products, like ice creams, cakes, logs, and novelty items with the “Ice Cream House” logo. Products are packed in clamshells or cake trays with plastic dome covers in various sizes and styles and have an Ice Cream House label, as seen above. Recalled products are not labeled with lot or date codes.
| ITEM DISCRIPTION | DAIRY / PARVE | UNIT SIZE | UPC |
|---|---|---|---|
| Premium Sorbet 5 Liter / All flavors | parve | 1 PACK | Food Service |
| Premium Ice Cream 5 Liter SUGAR FREE / All flavors | dairy | 1 PACK | Food Service |
| Premium Ice Cream 5 Liter / All flavors | dairy / parve | 1 PACK | Food Service |
| Premium Sorbet Mix 4 gal. All flavors | parve | 1 PACK | Food Service |
| Trio Log Sorbet | parve | 1 PACK | 0-91404-15166-5 |
| Trio Log Ice Cream Dairy | dairy | 1 PACK | 0-91404-15137-5 |
| Trio Log Ice Cream Parve | parve | 1 PACK | 0-91404-15136-8 |
| 9” Ice Cream Pie Vanilla / Chocolate | dairy / parve | 1 PACK | 0-91404-15428-4 |
| 9” Ice Cream Pie Razzle | dairy / parve | 1 PACK | 0-91404-15112-2 |
| Premium Sorbet Trifle Medium | parve | 1 PACK | 0-91404-15164-1 |
| Premium Sorbet Trifle Small | parve | 1 PACK | 0-91404-15165-8 |
| 8′ Sorbet Cake Strawberry / Mango | parve | 1 PACK | 0-91404-15429-1 |
| 10” Sorbet 4 Layer Cake | parve | 1 PACK | 0-91404-15111-5 |
| 10′ Heart Cake | dairy / parve | 1 PACK | 0-91404-15171-9 |
| 10′ Hello Kitty Cake | dairy / parve | 1 PACK | 0-91404-15174-0 |
| 10″ Round Cake | dairy / parve | 1 PACK | 0-91404-15179-5 |
| Mini Heart Cake | dairy / parve | 1 PACK | 0-91404-15173-3 |
| Mini Round Cake | dairy / parve | 1 PACK | 0-91404-15182-5 |
| Mini Sorbet Cake Blueberry / Lime | parve | 1 PACK | 0-91404-15219-8 |
| Mini Sorbet Cake Strawberry / Mango | parve | 1 PACK | 0-91404-15132-0 |
| Heaven Layer Vanilla / Strawberry / Mocha / Vanilla | parve | 1 PACK | 0-91404-15184-9 |
| Tropical Flute / Pre-Cut 12 Slices | parve | 1 PACK | 0-91404-15243-3 |
| Adventures Twist / Pre-Cut 12 Slices | parve | 1 PACK | 0-91404-15244-0 |
| Mont Blanc D’zert Ice Cream / Pre-Cut 12 Slices | parve | 1 PACK / SINGLE | 0-91404-15247-1 |
| De’Lighting Frozen Dessert / Pre-Cut 12 Slices | parve | 1 PACK / SINGLE | 0-91404-15266-2 |
| {P} Cookies & Cream Roll Cake | parve | 1 PACK / SINGLE | 0-91404-15299-3 |
| {P} Strawberry Shortcake Roll | parve | 1 PACK / SINGLE | 0-91404-15298-0 |
| 6′ Heart Cake | dairy / parve | 1 PACK | 0-91404-15172-6 |
| 6′ Hello Kitty Cake | dairy / parve | 1 PACK | 0-91404-15176-4 |
| {P} 6′ Round Cake | dairy / parve | 1 PACK | 0-91404-15181-8 |
| 6” Razzle Bomb | dairy / parve | 1 PACK | 0-91404-15422-2 |
| 6″ Sorbet Cake Passion Pomegranate | parve | 1 PACK | 0-91404-15155-9 |
| 8″ Square Vanilla Mocha Strawberry | parve | 1 PACK | 0-91404-15143-6 |
| 8′ Heart Cake | dairy / parve | 1 PACK | 0-91404-15309-6 |
| 8′ Hello Kitty Cake | dairy / parve | 1 PACK | 0-91404-15175-7 |
| 8″ Round Cake | dairy / parve | 1 PACK | 0-91404-15180-1 |
| 8” Razzle Bomb | dairy / parve | 1 PACK | 0-91404-15421-5 |
| Check’ice board Ice Cream Pre-Cut 12 Slices | dairy / parve | 1 PACK / SINGLE | 0-91404-15144-3 |
| Check’ice board Sorbet Pre-Cut 12 Slices Straw/Mango/Van | parve | 1 PACK / SINGLE | 0-91404-15144-3 |
| Car Cake large | dairy / parve | 1 PACK | 0-91404-15423-9 |
| Car Cake Small | dairy / parve | 1 PACK | 0-91404-15425-3 |
| 10” Sorbet Cake cherry | parve | 1 PACK | 0-91404-15111-5 |
| Ocean Waves | dairy / parve | 5 PACK / SINGLE | 0-91404-15300-3 |
| Cream ‘N’ Sorbet Pizzazz Mango | parve | 4 PACK / SINGLE | 0-91404-15140-5 |
| Cream ‘N’ Sorbet Pizzazz Strawberry | parve | 4 PACK / SINGLE | 0-91404-15141-2 |
| French Coffee Oval | dairy / parve | 4 PACK / SINGLE | 0-91404-15360-7 |
| Black ‘N’ Whites Vanilla Chocolate | dairy / parve | 6 PACK / SINGLE | 0-91404-15260-0 |
| Sorbet Swirl | parve | 6 PACK / SINGLE | 0-91404-15400-0 |
| Double Fudge Sandwich | dairy / parve | 6 PACK / SINGLE | 0-91404-15240-2 |
| Mini Cigars | dairy / parve | 10 PACK / SINGLE | 0-91404-15120-7 |
| Cigar Shells | dairy / parve | 6 PACK / SINGLE | 0-91404-15130-6 |
| Mini Cone | dairy / parve | 6 PACK / SINGLE | 0-91404-15220-4 |
| Mini Ice Cream Lollies | dairy / parve | 12 PACK / SINGLE | 0-91404-15110-8 |
| Mini Sorbet Lollies | parve | 12 PACK / SINGLE | 0-91404-15246-4 |
| Kleina Bites | parve | 12 PACK / SINGLE | 0-91404-15148-1 |
| Hearty Tart | parve | 6 PACK / SINGLE | 0-91404-15363-8 |
| Mister Cone | dairy / parve | 6 PACK / SINGLE | 0-91404-15430-7 |
| Sushi ‘N’ Cream | parve | 8 PACK / SINGLE | 0-91404-15291-4 |
| Mini Razzle ‘N’ Dazzle | dairy / parve | 9 PACK / SINGLE | 0-91404-15409-3 |
| Mini Sorbet | parve | 9 PACK / SINGLE | 0-91404-15408-6 |
| Rosebuds | parve | 5 PACK / SINGLE | 0-91404-15185-6 |
| Mini Chocolate Sorbet Tarts | parve | 12 PACK / SINGLE | 0-91404-15411-6 |
| Strawberry Himalaya | parve | 6 PACK / SINGLE | 0-91404-15135-1 |
| Peanut Butter Core | parve | 6 PACK / SINGLE | 0-91404-15134-4 |
| Trimocha Vanilla | dairy / parve | 6 PACK / SINGLE | 0-91404-15229-7 |
| Triangle Up Strawberry Mango Vanilla | parve | 6 PACK / SINGLE | 0-91404-15308-9 |
| Blossoming Daisies | parve | 6 PACK / SINGLE | 0-91404-15154-2 |
| Viennese Crunch Bites | parve | 10 PACK / SINGLE | 0-91404-15262-4 |
| Mini Roll Cake Assorted | parve | 8 PACK / SINGLE | 0-91404-15350-8 |
| Cup Cake Party | dairy / parve | 6 PACK / SINGLE | 0-91404-15287-7 |
| Mini Sorbet Pops | parve | 7 PACK / SINGLE | 0-91404-15305-8 |
| Biscoloti Dessert Cups | parve | 6 PACK / SINGLE | 0-91404-15311-9 |
| Coffee Dessert Cups | parve | 6 PACK / SINGLE | 0-91404-15313-3 |
| Smores Dessert Cups | parve | 6 PACK / SINGLE | 0-91404-15312-6 |
| Tiramisu Dessert Cups | parve | 6 PACK / SINGLE | 0-91404-15314-0 |
| Mini Dippers Ice Cream | parve | 6 PACK / SINGLE | 0-91404-15289-1 |
| Mini Sorbet Dippers | parve | 6 PACK / SINGLE | 0-91404-15303-4 |
| Frubic Scube | parve | 6 PACK / SINGLE | 0-91404-15301-0 |
| Kremlin’s | parve | 6 PACK / SINGLE | 0-91404-15302-7 |
| Mini Strawberries | parve | 12 PACK / SINGLE | 0-91404-15304-1 |
| Frozen Squares | dairy / parve | 4 PACK / SINGLE | 0-91404-15338 |
| Dessert on Wheels | dairy / parve | 4 PACK / SINGLE | 0-91404-15339-3 |
| Premium Sundae Quart / Chocolate Fudge | dairy / parve | 1 PACK | 0-91404-15340-9 |
| Premium Ice Cream Quart / Vanilla Fudge | dairy / parve | 1 PACK | 0-91404-15340-9 |
| Premium Ice Cream Quart / Vanilla Razzle | dairy / parve | 1 PACK | 0-91404-15161-0 |
| Premium Sorbet Quart / Blueberry Lime | parve | 1 PACK | 0-91404-15162-7 |
| Premium Sorbet Quart / Mango | parve | 1 PACK | 0-91404-15162-7 |
| Premium Sorbet Quart / Strawberry | parve | 1 PACK | 0-91404-15162-7 |
| Premium Sorbet Quart / Strawberry Mango | parve | 1 PACK | 0-91404-15162-7 |
| Premium Sorbet Quart / Trio / Vanilla Strawberry Mango | parve | 1 PACK | 0-91404-15162-7 |
| Premium Sunday Quart / Caramel Fudge | Dairy / parve | 1 PACK | 0-91404-15340-9 |
Products involved in the recall should be discarded or returned to the original point of purchase for a full refund or replacement.
“Ice Cream has a long shelf life and may still be in the freezers of consumers. Consumers should check their freezers and throw away the recalled ice cream products or return it to the place of purchase,” according to the recall notice.
Anyone with questions or concerns can email the company at: [email protected] or call 845-445-7644.
About Listeria infections
Food contaminated with Listeria monocytogenes may not look or smell spoiled but can still cause serious and sometimes life-threatening infections. Anyone who has eaten any recalledproducts and developed symptoms of Listeria infection should seek medical treatment and tell their doctors about the possible Listeria exposure.
Also, anyone who has eaten any of the recalled products should monitor themselves for symptoms during the coming weeks because it can take up to 70 days after exposure to Listeria for symptoms of listeriosis to develop.
Symptoms of Listeria infection can include vomiting, nausea, persistent fever, muscle aches, severe headache, and neck stiffness. Specific laboratory tests are required to diagnose Listeria infections, which can mimic other illnesses.
Pregnant women, the elderly, young children, and people such as cancer patients who have weakened immune systems are particularly at risk of serious illnesses, life-threatening infections, and other complications. Although infected pregnant women may experience only mild, flu-like symptoms, their infections can lead to premature delivery, infection of the newborn, or even stillbirth.
(To sign up for a free subscription to Food Safety News,click here)
]]>The issue was reported to FSIS after the ground beef product was submitted to a third-party laboratory for microbiological analysis and the sample tested presumptive positive for E. coli O157:H7.
The fresh ground beef products were produced on Aug. 22, 2023.
FSIS is concerned that some product may be in restaurant refrigerators or freezers.
These items were shipped to restaurant locations in the greater San Antonio, TX area.
Recalled products:
- 1-lb., 5-lb., and 10-lb. vacuum-sealed plastic bags containing “Peeler Farms WAGYU BEEF GROUND BEEF” with lot code 17836 represented on the label.
- 5-lb. vacuum-sealed plastic bags containing “R-C RANCH TEXAS CRAFT MEATS WAGYU RC13610 STEAKHOUSE BLEND – GROUND BEEF 5 lb” with lot code 17816 represented on the label.
- 8-oz. vacuum-sealed plastic bags containing “R-C RANCH TEXAS CRAFT MEATS WAGYU RC13603 – GROUND BEEF PATTIES 8 oz” with lot code 17816 represented on the label.
The products subject to recall bear establishment number “EST. 51283” inside the USDA mark of inspection.
As of the posting of this recall, there have been no confirmed reports of adverse reactions due to consumption of these products.
Restaurants are urged not to serve these products. These products should be thrown away or returned to the place of purchase.
About E. coli infections
Anyone who has eaten any of the implicated products and developed symptoms of E. coli infection should seek medical attention and tell their doctor about their possible food poisoning. Specific tests are required to diagnose the infections, which can mimic other illnesses.
The symptoms of E. coli infections vary for each person but often include severe stomach cramps and diarrhea, which is often bloody. Some patients may also have a fever. Most patients recover within five to seven days. Others can develop severe or life-threatening symptoms and complications, according to the Centers for Disease Control and Prevention (CDC).
About 5 to 10 percent of those diagnosed with E. coli infections develop a potentially life-threatening kidney failure complication, known as a hemolytic uremic syndrome (HUS). Symptoms of HUS include fever, abdominal pain, feeling very tired, decreased frequency of urination, small unexplained bruises or bleeding, and pallor.
Many people with HUS recover within a few weeks, but some suffer permanent injuries or death. This condition can occur among people of any age but is most common in children younger than five years old because of their immature immune systems, older adults because of deteriorating immune systems, and people with compromised immune systems such as cancer patients.
People who experience HUS symptoms should immediately seek emergency medical care. People with HUS will likely be hospitalized because the condition can cause other serious and ongoing problems such as hypertension, chronic kidney disease, brain damage, and neurologic problems.
(To sign up for a free subscription to Food Safety News, click here.)
]]>Scientists said findings can help guide and allocate public resources to prevent Bacillus cereus foodborne cases.
Data from 2010 to 2020 came from the National Foodborne Disease Outbreak Surveillance System.
A total of 419 Bacillus cereus outbreaks were reported, leading to 7,892 cases, 2,786 hospital admissions, and five fatalities. The bulk of outbreaks were recorded in summer, primarily between May and September, found the study published in China CDC Weekly.
Link to rice products and schools
The most recurrent food vehicle was connected with rice or flour-based products, notably those made with rice or fried rice and school canteens bore the brunt of outbreaks. This suggests contamination and improper storage during food preparation. So, it is essential to prioritize education for canteen staff on food safety and proper practices, said researchers.
“Given the difficulties students face in discerning food quality and the inherent nature of communal dining in schools, they are at a heightened risk for foodborne disease outbreaks. Therefore, to mitigate the frequency of such outbreaks, supervisory bodies should enhance their oversight and management of food safety in school canteens.”
Bacillus cereus produces toxins that can be classified into vomiting-type and diarrhea-type enterotoxins based on the symptoms they cause. Foodborne infections manifest with symptoms such as nausea, vomiting, and diarrhea.
The most outbreaks occurred in 2018 with 56 while 2012 had the most cases. The peak hospitalization rate was in 2011. One death occurred in 2014 and two each in 2015 and 2016.
Foods derived from rice or flour were identified as the primary cause of most outbreaks and associated cases. Bakery products were responsible for the highest hospitalization rate. Five deaths were traced to rice or flour-based products and complex foods. Rice and rice products accounted for more outbreaks than flour and flour products.
The primary source of these outbreaks, as well as related cases, was school cafeterias. However, the household setting had the highest hospitalization rate and mortality rate.
Factors behind outbreaks
Multifactor contamination was identified as the leading cause for outbreaks and associated cases. This was closely followed by improper storage, accounting for 111 outbreaks and 1,981 cases. The highest rate of hospitalization was attributed to food mishandling and ingestion errors.
In the multifactor classification, the occurrence of two factors was most prevalent. The most frequent combination was inadequate storage and inappropriate processing followed by ingredient contamination or spoilage with improper storage.
To mitigate the risk of Bacillus cereus outbreaks, it is essential to address a multitude of core control and management factors, said researchers.
“These include utilizing safe food ingredients, ensuring cleanliness and standardization throughout the food processing procedure, preventing cross-contamination, thoroughly cooking the food, among others. Implementing proper preservation to inhibit the growth of Bacillus cereus is of great significance.”
(To sign up for a free subscription to Food Safety News, click here.)
]]>Recent modifications to FDA’s import alerts, as posted by the agency, are listed below.
Click here to go to the FDA page with links to details on specific alerts.

(To sign up for a free subscription to Food Safety News,click here)
]]>